|
Finding the most effective and efficient way to treat patellofemoral pain has been a goal of physical therapists and orthopedic surgeons for years. Traditional bracing and surgery have proven to be inconsistent in providing pain relief, so many people with patellofemoral dysfunction (PFD) endure pain on a regular basis with no treatment options but to modify their activity, grin and bear it.
It is estimated that every year 13 million people visit their doctor with knee pain, of those 3.5 million are diagnosed with PFD. And, of the 3.5 million who are diagnosed with PFD, 3.2 million of them have a bony malalignment or patellofemoral malalignment. Patellofemoral dysfunction can be aggravated by insufficient quadriceps strength, increased femoral rotation, postural malalignments, and soft-tissue changes. Most often, people with patellofemoral dysfunction experience pain when going down stairs, squatting, during prolonged sitting and when rising from sitting and vigorous sports activities. The reason these movements or conditions are painful is because people are eccentrically loading the knee joint. This can put three to seven times your body weight of pressure on the patella. The patella can track poorly for a long period of time before the improper mechanics take their toll. However, once the pain and low grade inflammation develop it is difficult to reverse. People with patellofemoral pain generally have one of four patellar malalignments as shown in the diagram above. Tilt: Patellar tilt is typically toward the outside or lateral side of the leg. When lateral tilt occurs, the surface of the kneecap is at an abnormal angle at the end of the femur. As a result, the kneecap rides over the outside edge of the bony prominence of the femur resulting in wearing down of the kneecap cartilage. One of the symptoms of tilt is a weakened Vastus Medialis Oblique (VMO) muscle. Since the VMO is essential to keeping the patella tracking correctly, its lack of strength will contribute to an even greater malalignment. Glide: With a glide condition, the entire kneecap is shifted to the outside of the joint. Glide can be seen by comparing the inside and outside portions of the kneecap to its position relative to the femur. Once again, a glide condition will cause irritation to the underside of the patella and the surface of the femur bone. A/P: Anterior/Posterior malalignment occurs when the lower edge of the kneecap is tilted downward toward the tibia. The lower edge of the kneecap becomes buried in the fat pad below the patella and puts pressure on the patellar tendon. This can result in pain centered at the lower edge of the kneecap, irritation to the fat pad and inflammation of the patellar tendon. Rotation: In a knee with rotation malalignment, the kneecap’s midline is not parallel to the longitudinal axis of the femur. Rotation of the kneecap can result in wear and tear on the patellar cartilage and a disadvantaged kneecap position which will inhibit the VMO muscle’s ability to contract. Current treatments for patellofemoral dysfunction range from therapeutic exercise to strengthen the quadriceps, taping, bracing, and surgery. Therapeutic exercise and taping have their merits if the patient does NOT have one or more of the four malalignments addressed above. Exercise can serve to strengthen weak or de-conditioned quadriceps muscles and taping can effectively address soft tissue challenges. The best orthopedic surgeons do not operate until all means of physical therapy have been exhausted. In some cases, surgery may be an option. There are two surgeries commonly performed to do patellar realignments. The less invasive measure is an arthroscopic surgery in which the lateral retinaculum is released by being cut, with the hope that it will stop pulling on the patella, thus allowing it to find its anatomically correct location. It is paramount that physical therapy is started day-1 post-op in order to eliminate the swelling in the knee joint and to ensure that the lateral retinaculum does not scar down. The second surgical method often selected is and open procedure called an extensor mechanism realignment. This process entails lifting the patellar tendon off the tibia at the tibial tubercle where the tendon attaches. The tendon is then moved medially and stapled back to the bone (tibia). The second step of this surgery is to do a lateral release and then finally a VMO advancement. The VMO advancement involves cutting the VMO muscle off the patella and advancing it distally on the patella in an attempt to enhance the horizontal pull of the VMO fibers. This is an extensive surgery and requires approximately 6 to 8 months of post-op physical therapy. Physical therapists are the musculoskeletal and therapeutic exercise experts who can help the patellofemoral patients manage this very challenging malady. We as therapists must go beyond only taking someone’s pain away. We need to realize that we can have a profound effect on people’s lives by enabling them to perform activities and sports, or to pursue the careers of their dreams. As clinicians, we need to begin our treatment with this patient with a thorough evaluation and examination to identify the factors contributing to a patient’s PFD. It is also essential that we perform a comparable sign prior to treating our patients to determine the effectiveness of our chosen treatment method. A comparable sign reproduces the patient’s pain, and the treatment method must greatly alleviate or eliminate the patient’s pain. There are two things we must do for the PFD patient, and it is important that they are done in this order: 1) Realign the patella back in the interchondylar groove, put a constant stretch on the lateral retinaculum, and eliminate the pain cycle. 2) Then, in this pain-free environment, develop a thorough manual therapy and therapeutic exercise program to maximize the function of the quadriceps muscles, particularly the VMO. When these two steps are accomplished you will be successful in resolving PFD and returning your patients back to functional and athletic activities long-term. As discussed earlier, to date, treatment methods have been varied and clinical results have been inconsistent. Radiographic evidence, as well as positive patient response and clinical trials, have presented compelling evidence that knee pain caused by PFD can be reduced significantly or eliminated in most cases. Clinical trials were done with 35 subjects performing 10 functional activities with either no brace, a standard patellofemoral brace, or the OnTrack® System. Each subject was tested on three different occasions over an 8-week period. All subjects experienced a significant and, in many cases, a complete elimination of the patellofemoral knee pain when using the OnTrack System. The OnTrack treatment method reduces or eliminates pain immediately upon application by using a neoprene cuff, a neoprene strap, adhesive knee patches, and a VMO Activator Kit. Also included in the system is a patient educational DVD that explains patellar pain, the application of the OnTrack System, and the recommended exercises for rehabilitating knee-area muscles. The OnTrack treatment method was created to give clinicians and evidence-based tool that provides PFD patients immediate pain relief on day one, and allows you to progress them quickly and successfully through a treatment plan.
3 Comments
Kate just finished treating a patient who for the past 38 years has had a challenge with her kneecaps subluxing every single time she straightens either leg into full extension and when participating in low impact aerobics. Oftentimes when this happens she experiences swelling in her knee joint which leads to pain. She is a beautiful, active, intelligent woman who found her way to our clinic via a doctor who is in private practice, is progressive and seeks out professionals like Kate to treat his patients.
The good news regarding this patient is that Kate was able to help this woman by applying the OnTrack® Treatment Method on both knees. The woman broke down in tears because it was the first time in 38 years that she could move freely without her kneecaps subluxing and severely limiting her ability to be active and live a normal life. The bad news regarding this patient is that until now, not one medical professional from whom she sought help in the past 38 years correctly diagnosed and treated her knee malady. Although unpardonable, sadly this happens all too often. Patients frequently get caught up in a health care environment that can easily be compared to being up a creek without a paddle. They get lost in the chaos and no one takes the time to really listen to them or take good care of them. This happens more and more as medical professionals can no longer survive in private practice. They succumb to joining large, bureaucratic, medical entities where they are double or even triple booked with patients, regularly running an hour or more behind schedule and spending only a few unfocused minutes with each patient. If a patient needs physical therapy they are often sent to the clinic owned by the physician, which is allegedly illegal in California. Or, the doctor will send them to a clinic that forces its’ therapists to see 4-6 patients per hour. In our humble opinion, neither of these options is appropriate or acceptable. No wonder people can bounce around for years without getting the help they so desperately need and deserve. The Chief of Staff at Scripps Memorial Hospital in La Jolla, CA recently said, “I have learned that all accomplishments are directly proportional to the interest and passion each person contributes to getting “stuff” done.” We agree whole heartedly with this. At Kate Grace Physical Therapy we pride ourselves on getting “stuff” done. It is NOT, nor will it ever be okay with us for a patient to live a compromised life for 38 years before getting good care. Our patients will not sit in our lobby waiting to be seen. Our therapists stay on-time all day, every day. Our patients will be educated by our therapists so that they understand what is wrong with them and how we are going to fix it. Our patients will be better after every visit. We will invite each of our patients to advance their level of health beyond what it was when we met them. And we will facilitate them in achieving this if they want our help. We ask that you keep this in mind when you, a family member, friend, or co-worker needs medical attention. You have a bunch of interested and passionate people whose primary goal is to make a positive contribution to people like you every day. Call us, we can and will help! It seems as though the entire planet has been consumed with World Cup fever the past few weeks, and for good cause. This year's tournament is living up to its' high expectations. The United States' first group win since 1930, and many upsets, including defending champs not even emerging from group play!
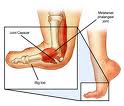
While there have been great moments, there have also been some not so great moments. Many people cannot get the hive of bees, I mean vuvuzelas, from ringing in their ears for hours after the games are already over. Not to mention blown calls by referees; reversing goals from players called offsides when they weren't, and not counting goals that were good by at least 3-4 feet. However, for many, the worst part of the World Cup is all of the FLOPPING! Soccer players are notorious for flailing their bodies about at the very threat of contact, attempting to get a call in their favor. It seems that a lot of these soccer players could have quite the career on Broadway after they retire from the pitch. However, while at times these players will fake and injury, many of these great athletes push through painful injuries that would keep most of us off of the field. One of the painful injuries that plague soccer players from the World Cup to high school and recreational team fields is the dreaded Turf Toe. Turf toe is an injury to the big toe when it is extended upward with high force. This injury often occurs in athletes who play soccer, football, and rugby. Turf toe received its name due to the large number of these injuries happening on artificial turf or surfaces. Turf toe typically occurs when an athletes shoe sticks to the turf while their bodyweight continues to go forward, causing the toe to hyperextend upward. Turf toe usually presents with pain and inflammation at the base of the big toe, or 1st metatarsal joint. Pain with flexion or extension of the big toe is another common symptom. If the injury is severe enough, the ligaments and bone on the bottom of the big toe can be damaged. Turf toe sprains are categorized by 3 grades. Grade 1 is accompanied by mild pain, but not limiting a player from competition. Grade 2 can cause an athlete to have to rest 3-14 days, while Grade 3 injuries can cause missed playing time of 2-6 weeks. Treatment of turf toe is variable based on the grade of injury. All injuries are acutely treated with rest, ice, compression, and elevation (RICE), as well as non-steroidal anti-inflammatory drugs (NSAIDS). Crutches are used for more severe sprains to allow the joint to heal without weight bearing. Your physical therapist can assist with further treatment through taping the joint to prevent motion. Therapeutic modalities such as ultrasound may be used to help increase the rate of healing. Typically, around 3-5 days after injury, pain free range of motion activities are initiated. All grades of injury can benefit from a rehabilitation and strengthening program developed by a physical therapist. Physical therapy plays an important role in recovery and prevention of hallux limitus (the development of arthritis in the joint, thereby decreasing range of motion). One hallux limitus is developed, it can have a lasting effect on gait mechanics, leading to further injuries in other joints of the lower extremeties. So as you watch the rest of the World Cup and happen to see a player flip into the air from tripping over an imaginary line...just remember, real injuries CAN actually happen without contact. |
Quote of the Day"You are always only one choice away from changing your life." Archives
April 2023
|
San Diego, CA 92121 Fax: (858) 457-0976 M - F: 6:45 am - 7:00 pm
Email: [email protected]


 RSS Feed
RSS Feed